Top Digestive Health Drugs for Gastrointestinal Disorders

Key Highlights
- Maintaining good digestive health is crucial for your overall well-being and quality of life.
- Digestive medications are widely used to manage conditions but can have common side effects.
- Proper gastrointestinal care involves understanding both the benefits and risks of these drugs.
- Many medications work by controlling stomach acid, but long-term use requires caution.
- Over-the-counter drugs are accessible, but persistent issues warrant a visit to a healthcare provider.
- Lifestyle choices like diet and exercise play a significant role in preventing digestive problems.
Introduction
Your digestive system is the engine that fuels your body, but for millions of Americans, it doesn’t always run smoothly. Reports show that over 60% of people in the U.S. experience regular gastrointestinal (GI) distress, with many finding their lives disrupted by digestive disorders. While a range of medications can offer relief, it is important to understand how they work. This guide provides a closer look at digestive health, common issues, and the healthcare options available to keep your GI tract in top shape.
Overview of Digestive Health and Medication Use in the United States
In the United States, digestive health issues are incredibly common, affecting a significant portion of the adult population. With so many people experiencing GI issues that impact their quality of life, the use of digestive medications has become widespread. These drugs, from simple antacids to powerful prescription therapies, are designed to soothe the digestive tract and restore normal function.
While these medications provide much-needed relief, they are not without risks. Understanding the proper use of digestive medications, their potential side effects, and when to seek professional advice is key to managing your gut health effectively. We will explore the different types of drugs, how they work, and what you need to know to use them safely.
Key Functions of the Digestive System
Your digestive tract does much more than just process the food you eat. When it’s working correctly, it efficiently absorbs essential nutrients that your body needs for energy and daily functions. A healthy gut is the foundation of overall wellness, supporting everything from your immune system to your mental clarity.
One of the clearest signs of good gut health is having regular bowel movements without pain, bloating, or gas. This indicates that your system, from your stomach lining to your small intestine, is functioning as it should. Any disruption in this process can throw your entire body off balance, highlighting why maintaining digestive wellness is so important.
Ultimately, the goal is to have a digestive system that works smoothly without you having to think about it. When your body effectively digests food and absorbs nutrients, you feel more energetic and balanced. This seamless operation is a hallmark of a healthy gut and a key component of a vibrant life.
Factors Affecting Digestive Health
Many factors can disrupt your digestive health, some of which are tied to modern lifestyles. The American diet, often low in fiber, along with sedentary habits and rising obesity rates, can contribute to problems like constipation and abdominal pain. Your individual gut microbiome is also a critical factor, as imbalances can lead to a variety of GI issues.
Certain trends may also explain the rise in digestive problems. For instance, frequent antibiotic use can alter your gut’s delicate balance, while increased anxiety and depression are closely linked to gut-brain disorders like IBS. These factors can create an increased risk for digestive distress.
Other key contributors to poor digestive health include:
- Insufficient water intake
- Not eating enough vegetables
- High levels of stress
- Taking certain medications
Each of these can affect everything from the amount of acid in your stomach to your ability to have regular bowel movements, potentially leading to a need for medications to manage these functional gastrointestinal disorders.
Role of Medications in Gastrointestinal Care
GI medications play a vital role in managing digestive disorders, offering relief from pain and discomfort. For many, these drugs are essential for improving quality of life and can even be lifesaving. They work in various ways, such as neutralizing stomach acid, reducing inflammation, or promoting the healing of ulcers to restore normal digestive function.
However, all digestive medications come with the potential for adverse effects. This can be particularly true for drugs used long-term, as your body might develop a dependency on them to function properly. For example, overuse of certain laxatives can weaken natural bowel activity over time.
It is crucial to use these medications wisely. Some GI medications can even cause other digestive symptoms, creating a cycle of treatment. Consulting with a healthcare professional helps ensure you are using the right drug for your condition and are aware of any potential risks involved.
Common Digestive Disorders and Their Drug Treatments
Digestive disorders range from mild discomfort to serious chronic conditions. Common issues include acid reflux (GERD), irritable bowel syndrome (IBS), inflammatory bowel disease (IBD), and peptic ulcers. Any pain or blockage along the GI tract could indicate an underlying problem that requires treatment.
Fortunately, most of these conditions can be managed effectively with medication. Each disorder has specific drug treatments designed to relieve symptoms, address the root cause, and prevent complications. The following sections will cover the pharmacological approaches for some of the most prevalent digestive issues, highlighting their benefits and potential side effects.
Managing Indigestion and Heartburn
Indigestion and heartburn are often caused by acid reflux, a condition where stomach acid flows back into the esophagus. This creates a burning sensation and discomfort. If this reflux becomes frequent, it’s known as gastroesophageal reflux disease (GERD), which can lead to more serious issues if left untreated.
Several types of medications are used to manage these symptoms by controlling stomach acid. An antacid offers quick, temporary relief by neutralizing existing acid. For more persistent issues, H2 blockers and proton pump inhibitors (PPIs) work by reducing the amount of acid your stomach produces.
Common symptoms that these medications help manage include:
- A burning feeling in the chest (heartburn)
- Regurgitation of food or sour liquid
- Difficulty swallowing
- Persistent upper abdominal discomfort
Choosing the right medication depends on the frequency and severity of your symptoms.
Medications for Irritable Bowel Syndrome (IBS)
Irritable bowel syndrome (IBS) is a chronic disorder affecting the large intestine. It causes symptoms like abdominal pain, bloating, and changes in bowel movements, such as diarrhea or constipation. Since the exact cause is often unknown, treatment for these GI issues typically focuses on managing symptoms.
For individuals with IBS-related diarrhea and cramping, prescription medications like dicyclomine can be effective. This drug works by blocking receptors in the GI tract that cause muscle spasms, thereby reducing pain and discomfort. It is considered relatively safe, with common side effects including dry mouth and constipation.
Managing IBS often involves a combination of lifestyle changes and medication. Since triggers can include stress, certain foods, and hormonal shifts, identifying and avoiding them is a key part of the treatment plan. Working with a doctor can help you find the right approach to control your symptoms and improve your quality of life.
Drug Options for Inflammatory Bowel Disease (IBD)
Inflammatory bowel disease (IBD) refers to serious conditions like Crohn’s disease and ulcerative colitis, which cause chronic inflammation in the digestive tract. Unlike IBS, IBD involves visible damage to the intestines, leading to symptoms like diarrhea, bloody stools, and abdominal pain.
Treatment for IBD aims to reduce inflammation, promote the healing of ulcers, and improve a person’s quality of life. Mesalamine is often considered a first-line treatment for mild IBD, particularly ulcerative colitis, as it works directly in the gut to reduce inflammation. While most people tolerate it well, some may experience GI upset.
Another common medication is budesonide, an oral steroid that calms inflammation in the colon. Its unique feature is that it is metabolized by the liver before entering systemic circulation, which means it has fewer side effects than other steroids. These drugs are key components in managing IBD and preventing long-term complications.
Pharmacological Approaches for Gastritis and Ulcers
Gastritis (inflammation of the stomach lining) and peptic ulcers (sores in the stomach or small intestine) are often caused by a bacterial infection called Helicobacter pylori or long-term use of NSAIDs like ibuprofen. These conditions cause stomach pain, bloating, and discomfort.
Pharmacological treatments focus on reducing stomach acid and protecting the stomach lining to allow it to heal. Stomach acid medications like proton pump inhibitors (PPIs) and H2 blockers are highly effective because they decrease acid production, which alleviates irritation. Another drug, sucralfate, works by forming a protective barrier over the ulcer, shielding it from acid.
These drug options provide a multi-faceted approach to healing. Below is a summary of common treatments for gastritis and ulcers:
| Drug Category | How It Works |
|---|---|
| Proton Pump Inhibitors (PPIs) | Block the enzyme that creates stomach acid, effectively stopping production. |
| H2 Blockers | Bind to receptors that trigger acid release, reducing overall acid levels. |
| Sucralfate | Creates a protective coating over the ulcer or inflamed area to promote healing. |
| Antibiotics (for H. pylori) | Eradicate the bacterial infection that is causing the ulcer. |
Types of Digestive Health Drugs Available
A wide variety of digestive medications are available to address different GI issues. These drugs are broadly categorized based on how they work, from a simple antacid that offers immediate relief to more complex GI medications that target specific biological processes.
Understanding these categories can help you make more informed decisions about your health. The following sections will break down common types of drugs, including acid blockers, laxatives, and GI stimulants. We will explore what they are used for, how they function, and what you should know before taking them.
Acid Reducers: Antacids, H2 Blockers, and Proton Pump Inhibitors
Acid reducers are among the most commonly used drugs for digestive issues like heartburn, GERD, and ulcers. They work by either neutralizing or decreasing the production of stomach acid. An antacid, which often contains calcium carbonate, provides quick relief by directly neutralizing acid in the stomach.
H2 blockers and proton pump inhibitors (PPIs) offer a more proactive approach. H2 blockers reduce acid production by blocking histamine signals, while PPIs are even more powerful, shutting down the pumps that release acid into the stomach. These are often recommended for more chronic conditions.
Here are some common examples:
- Antacids: Tums, Rolaids
- H2 Blockers: Pepcid (famotidine), Tagamet (cimetidine)
- PPIs: Prilosec (omeprazole), Nexium (esomeprazole)
While effective, long-term use of PPIs has been linked to potential risks, so it is important to use them under a doctor’s guidance.
Laxatives and Stool Softeners for Constipation
When you are dealing with constipation, laxatives and stool softeners can help restore regular bowel movements. These medications work in different ways to make it easier to pass stool. Some, like bulk-forming fibers, add volume to your stool, while others, known as osmotics, draw water into the colon to soften it.
Over-the-counter options are widely available, but it is important to use them correctly. For example, some antacids containing magnesium hydroxide can act as a laxative, while those with aluminum hydroxide may cause constipation. Stronger prescription laxatives are also available for more severe cases.
Experts caution against the long-term use of certain laxatives, especially stimulants like senna, as they can lead to dependency and weaken natural bowel function. Overuse can also cause dehydration and nutrient imbalances. Therefore, they should be used as a short-term solution while you work on lifestyle changes like increasing fiber and water intake.
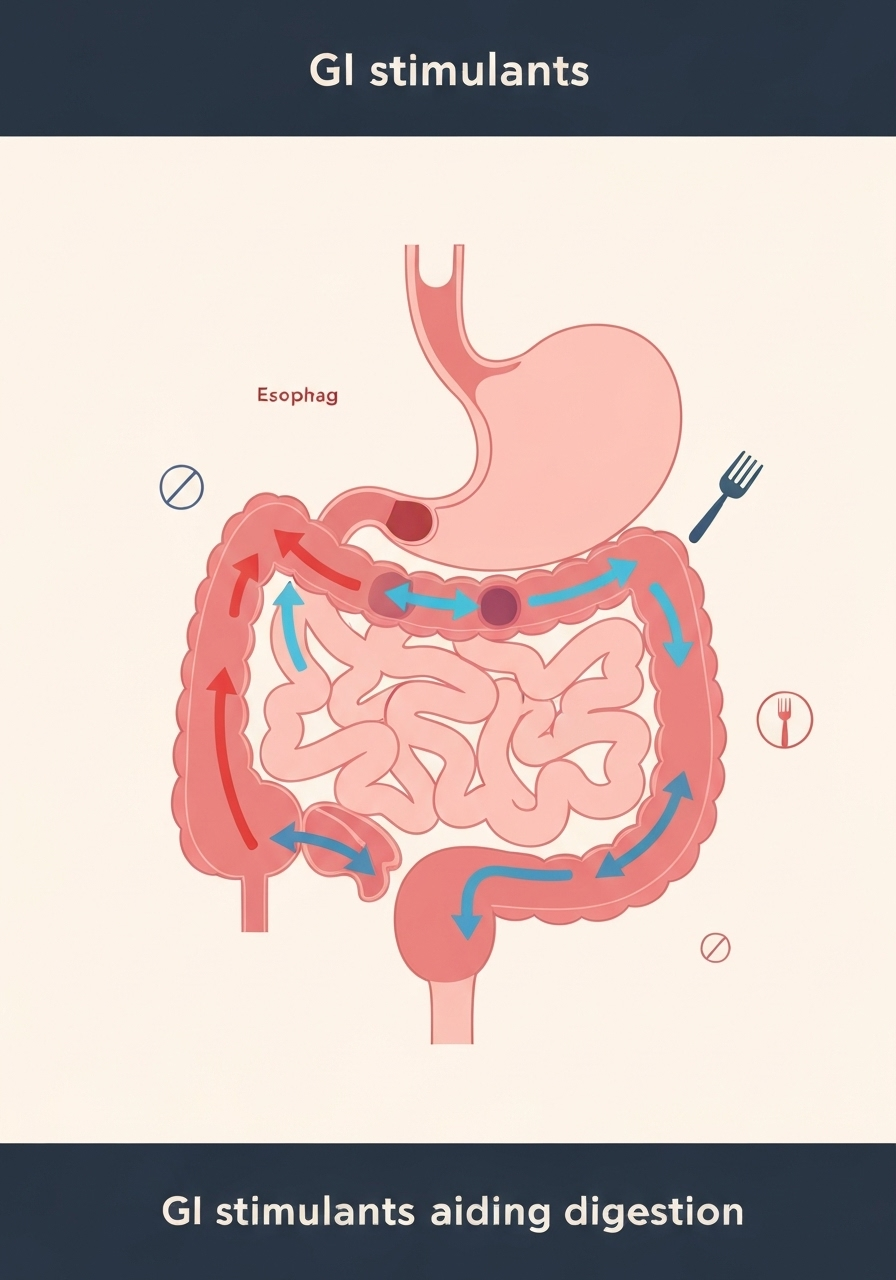
GI Stimulants: Uses and Prescriptions
GI stimulants, also known as promotility agents, are prescription medications designed to help food move more quickly through the digestive tract. They are typically prescribed for conditions like gastroparesis (delayed stomach emptying) or as an anti-nausea treatment. These drugs work by enhancing the contractions of the muscles in the GI tract.
Metoclopramide is a widely used GI stimulant that helps relieve nausea and heartburn. It blocks certain brain signals that cause nausea and speeds up the movement of food through the stomach and intestines. It is available in various forms, including tablets.
While effective, these drugs can have serious side effects, especially with long-term use. The most concerning is a neurological disorder called tardive dyskinesia, which causes involuntary movements. For this reason, GI stimulants are usually prescribed for short durations and under close medical supervision to ensure safety while managing symptoms.
Other Therapeutic Agents: Sucralfate, Mesalamine, Budesonide
Beyond the more common categories, several other therapeutic agents target specific digestive issues. These drugs offer unique mechanisms of action for conditions like inflammatory bowel disease (IBD), gastritis, and ulcers.
Sucralfate, for example, is prescribed to treat an ulcer or inflammation by forming a protective layer over the affected area, shielding it from stomach acid and allowing it to heal. Mesalamine and budesonide are key drugs in managing IBD by directly targeting inflammation within the gut.
These agents are often part of a comprehensive treatment plan:
- Sucralfate: Creates a protective barrier to help heal an ulcer or gastritis.
- Mesalamine: Reduces inflammation in the gut, primarily for ulcerative colitis.
- Budesonide: A targeted steroid that decreases inflammation in the colon for Crohn’s disease and colitis.
These prescription medications are vital for managing chronic digestive diseases and improving patients’ quality of life.
Choosing Between Over-the-Counter and Prescription Digestive Medications
When you need relief from digestive issues, you will find both over-the-counter (OTC) and prescription medications available. The main difference lies in their accessibility and strength. OTC drugs are easy to purchase and are suitable for mild, occasional symptoms.
However, for persistent or severe problems, a prescription from a healthcare provider is necessary. A doctor can provide a proper diagnosis and prescribe a more potent medication tailored to your specific condition. The following sections will explore the differences in more detail and help you decide when it is time to seek professional medical advice.
Differences in Accessibility and Potency
The most obvious difference between over-the-counter and prescription drugs is accessibility. You can buy OTC medications at any pharmacy without a doctor’s note, making them convenient for immediate relief. Prescription drugs, on the other hand, require a consultation and a formal prescription from a healthcare professional.
This difference is directly related to their potency and potential for serious side effects. Prescription medications are typically stronger and designed to treat more complex or chronic conditions. Their use requires medical supervision to manage dosage and monitor for adverse reactions. OTC drugs are less potent, but long-term use without a diagnosis can mask a more serious underlying issue.
Here is a simple comparison:
| Feature | Over-the-Counter (OTC) | Prescription (Rx) |
|---|---|---|
| Accessibility | Available at most stores without a doctor’s note. | Requires a prescription from a healthcare provider. |
| Potency | Lower strength, for mild or occasional symptoms. | Higher strength, for chronic or severe conditions. |
| Supervision | Self-managed by the user. | Use is monitored by a healthcare professional. |
| Risk | Generally lower risk for short-term use. | Higher potential for side effects; requires monitoring. |
When to Seek a Prescription for Gastrointestinal Issues
While over-the-counter medications can handle minor digestive complaints, it is important to know when to consult a healthcare provider. If you experience persistent symptoms like chronic abdominal pain, unexplained weight loss, or bleeding, you should seek a professional diagnosis. These could be signs of a more serious condition that OTC drugs cannot treat.
A healthcare provider can determine the root cause of your issues and prescribe the appropriate treatment. Self-diagnosing and relying on OTC medications for long periods can be risky, potentially masking a problem or leading to complications. In rare cases, unchecked symptoms could be related to conditions like liver disease.
Furthermore, a doctor can help you navigate potential side effects and drug interactions. If you experience any unusual symptoms after starting a new medication, such as severe allergic reactions, it is crucial to get medical attention immediately. A prescription ensures you receive targeted, supervised care for your specific needs.
Conclusion
In summary, understanding digestive health drugs is crucial for effectively managing gastrointestinal issues. From over-the-counter solutions to prescription medications, knowing the right options for conditions like indigestion, IBS, and IBD can significantly enhance your quality of life. It’s important to consider not only the type of medication but also how it interacts with your body and lifestyle. As you navigate through your choices, don’t hesitate to seek advice from healthcare professionals who can guide you toward the best treatment tailored to your needs. If you’re interested in exploring digestive health solutions further, feel free to reach out for a free consultation.
Frequently Asked Questions
What are common side effects of digestive health drugs?
The most common side effects of digestive health drugs often involve further digestive upset. These adverse effects can include nausea, diarrhea, constipation, headaches, and loss of appetite. The specific side effects depend on the type of medication you are taking, so it is important to read the label carefully.
How do digestive medications interact with the body?
GI medications interact with the body in various ways. Some neutralize stomach acid directly, others reduce acid production, decrease inflammation, or coat the stomach lining to promote the healing of ulcers. The goal is to restore normal function and relieve symptoms by targeting a specific part of the digestive process.
What drug options are available specifically for treating gastritis?
For gastritis, treatment focuses on reducing acid and protecting the stomach. Common drug options include proton pump inhibitors (PPIs) and H2 blockers to decrease acid production. Agents like sucralfate or bismuth subsalicylate can also be used to coat and protect the stomach lining, allowing it to heal.
https://doi.org/10.1136/flgastro-2013-100316
https://doi.org/10.1186/1472-6904-11-2
https://www.nlm.nih.gov/medlineplus/druginfo/meds/a699060.html
https://medlineplus.gov/constipation.html
https://medlineplus.gov/hemorrhoids.html
https://pmc.ncbi.nlm.nih.gov/articles/PMC2855237
https://pubmed.ncbi.nlm.nih.gov/12973372
https://ods.od.nih.gov/factsheets/Probiotics-HealthProfessional