The Latest Obesity Drugs and Medication You Should Know
Key Highlights
- Newer obesity medications, like GLP-1 receptor agonists, have shown significant effectiveness in promoting weight loss.
- Eligibility for these prescription drugs typically requires a body mass index (BMI) of 30 or higher, or 27 with related health conditions.
- Medications like semaglutide (Wegovy) and tirzepatide (Zepbound) work by reducing appetite and making you feel full longer.
- Obesity is treated as a chronic disease, often requiring long-term medication use for sustained weight management.
- Combining these drugs with lifestyle changes, such as a healthy diet and physical activity, yields the best results.
- Common side effects include digestive issues, but more serious side effects are possible.
Introduction
Navigating the world of weight loss can be challenging, but recent advancements in medicine are offering new hope. If you’re dealing with obesity, you may have heard about the buzz surrounding the latest prescription drugs. These medications represent a significant shift in how we approach weight management, moving beyond just diet and exercise. This guide will walk you through the newest obesity drugs, explaining how they work, who they are for, and what you can expect on your journey to better health.
Understanding Obesity and Treatment Options
Obesity is more than just a number on a scale; it’s a complex medical issue defined by an excess amount of body fat. Doctors often use the body mass index (BMI) as a starting point to diagnose it. This condition can lead to various health conditions, making effective weight management crucial.
Fortunately, the treatment of obesity has evolved significantly. Beyond diet and exercise, a range of medical therapies is now available. These options provide another tool to help you manage your weight and improve your overall health. Let’s explore what defines obesity and the role of medication in its treatment.
What Defines Obesity and Why Medical Treatment Matters
Obesity is a medical condition characterized by an excessive amount of body fat that presents a risk to your health. A common tool used to screen for it is the body mass index (BMI). Generally, a BMI of 30 or higher is considered in the obese range. This can lead to serious health problems like heart disease and type 2 diabetes.
Because of these risks, medical treatment is often necessary. Prescription obesity medications are typically considered for individuals with a BMI of 30 or greater. They may also be an option for those with a BMI of 27 or higher who also have at least one weight-related health condition.
Deciding on medication involves a thorough discussion with your doctor about your medical history and the results from clinical trials. This ensures the chosen treatment is safe and appropriate for your specific needs, helping you on your path to a healthier weight.
Overview of Obesity Drug Therapy in the United States
The landscape of prescription weight loss in the United States has changed dramatically. For many years, options were limited. However, the FDA has approved several new medications, expanding the tools available for the treatment of obesity. This has brought a surge in public awareness and interest in drug therapy.
These medications are an important part of a comprehensive health care plan. A healthcare provider will consider your individual health profile, the medication’s cost, and potential side effects before prescribing. The drug administration method, whether an injection or a pill, is also a factor.
Currently, several medications are approved for weight management in the U.S. These include older drugs like phentermine and orlistat, as well as newer options like semaglutide (Wegovy), tirzepatide (Zepbound), and liraglutide (Saxenda), which have gained significant attention.
How Prescription Obesity Medications Work
Have you ever wondered how prescription obesity medications actually help you lose weight? These advanced weight loss drugs are designed to interact with your body’s natural systems that control hunger, fullness, and metabolism. They are a key part of a comprehensive weight management plan.
Instead of just relying on willpower, these prescription drugs provide a biological boost to help you manage your body weight more effectively. Understanding the science behind them can help you see why they’re becoming a popular choice for so many. Let’s look at the different ways these medications function.
Mechanisms Behind Weight Loss Drugs
Modern weight loss drugs use several clever mechanisms to achieve body weight reduction. They primarily target the neurohormonal pathways in your brain that regulate appetite and how full you feel. This helps you eat less without feeling constantly hungry.
Some of the most effective medications are known as receptor agonists. These drugs mimic hormones in your body that signal satiety, or fullness, to your brain. Initially developed for diabetes treatment, their powerful weight loss effects were quickly recognized. The main ways these drugs work include:
- Decreasing your appetite or reducing cravings.
- Helping you feel full with smaller meals.
- Slowing down how quickly your stomach empties.
By acting on these biological processes, these medications help lower your body’s “weight set point,” making it easier to lose weight and keep it off.
The Role of Hormones in Weight Loss Medications
Hormones play a starring role in the new generation of weight loss medications. Many of these drugs work by mimicking a hormone called glucagon-like peptide-1, or GLP-1. Your gut naturally produces GLP-1 after you eat, and it sends signals to your brain that you are full. It also helps control blood sugar.
By activating the same receptors as this natural hormone, medications like semaglutide and liraglutide help reduce your appetite and food intake, leading to weight loss. This is why many drugs initially used for diabetes treatment are now prescribed for obesity.
The most common prescription medications for treating obesity today often fall into this category of GLP-1 receptor agonists. Their ability to influence these key hormones makes them a highly effective tool for managing weight and improving metabolic health, moving beyond just calorie counting.
FDA-Approved Obesity Drugs: An Overview
When considering prescription weight loss medications, it’s essential to know which ones have received FDA approval. This seal of approval means the drug has undergone extensive clinical trials to prove it is both safe and effective for treating obesity and related health conditions.
The FDA sets a high bar for approval, ensuring that the benefits of a medication outweigh its potential risks. This process gives you and your doctor confidence in the treatment you choose. Let’s review the criteria for FDA approval and some of the common drugs that have met these standards.
Criteria for FDA Approval
For an obesity drug to get FDA approval, it must pass through rigorous testing. This process involves multiple phases of clinical trials where researchers evaluate the drug’s safety and effectiveness. The primary goal is to show that the medication can lead to significant weight loss compared to a placebo.
During these trials, the drug must demonstrate that its benefits for weight management are greater than its risks. The FDA looks for an average weight loss of at least 5% more than a placebo group over one year. Safety is a top priority, so any potential side effects are closely monitored and reported.
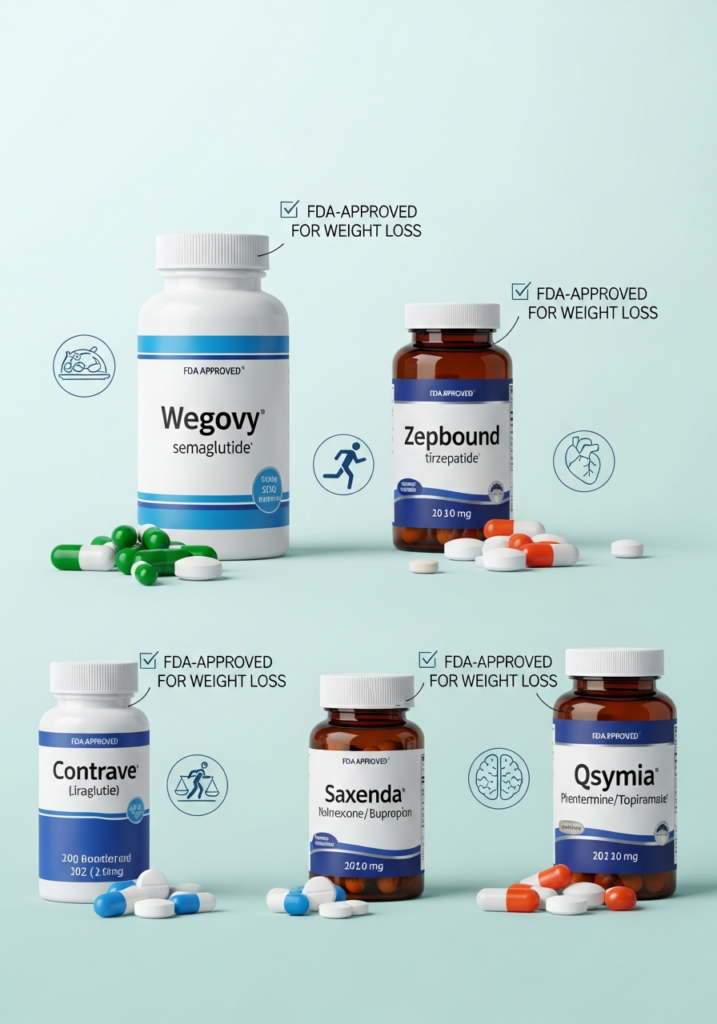
Once a drug meets these strict standards, it can be integrated into a patient’s treatment plan. The FDA has approved several medications for long-term weight management, including Wegovy, Zepbound, Saxenda, Qsymia, and Contrave, giving patients and doctors a range of evidence-based options.
Common Prescription Medications for Treating Obesity
There is a growing list of prescription drugs available to help you manage your body weight. These weight loss medications work in different ways and are selected based on your individual health needs. Your doctor can help you decide which brand name might be the best fit for you.
Newer medications like GLP-1 agonists have become very popular due to their high effectiveness. However, older options are still widely used and can be a good choice, especially when cost is a concern.
Here are some of the most common prescription medications for treating obesity:
| Drug Name | Brand Name(s) | How It’s Administered |
|---|---|---|
| Semaglutide | Wegovy, Ozempic | Weekly Injection or Daily Pill |
| Tirzepatide | Zepbound, Mounjaro | Weekly Injection |
| Liraglutide | Saxenda | Daily Injection |
| Phentermine-topiramate | Qsymia | Daily Capsule |
| Naltrexone-bupropion | Contrave | Daily Tablet |
GLP-1 Medications for Obesity
A specific class of drugs, known as GLP-1 receptor agonists, has revolutionized weight loss treatment. These medications were originally developed for diabetes treatment but were found to be incredibly effective for helping people lose weight and reduce their body mass.
GLP-1 drugs work by mimicking a natural hormone that targets areas of the brain involved in appetite regulation. This makes you feel fuller longer and reduces your desire to eat. Let’s take a closer look at some popular GLP-1 drugs and how they achieve such impressive results.
Popular GLP-1 Drugs: Semaglutide and Tirzepatide
Among the most talked-about GLP-1 drugs are semaglutide and tirzepatide. Semaglutide, known by brand names like Wegovy and Ozempic, has received widespread attention for its powerful weight loss effects. It’s approved for adults with a high body mass index.
Tirzepatide, sold as Zepbound or Mounjaro, is even newer and works on two hormone receptors, GLP-1 and GIP. This dual-action mechanism has shown even greater weight loss in clinical trials, making it one of the most effective options available today. Both medications also help regulate blood sugar, providing an added benefit for many patients.
These GLP-1 drugs are highly effective tools for managing obesity. They are typically prescribed for individuals with a BMI of 30 or higher, or 27 and above with weight-related health issues, helping them achieve significant and sustained weight loss.
How GLP-1 Drugs Help With Weight Loss
GLP-1 prescription drugs are a game-changer for weight loss because they target the body’s natural appetite control system. They mimic the GLP-1 hormone, which is released after eating to signal fullness to your brain. This helps you feel satisfied with smaller portions and reduces overall calorie intake.
Beyond controlling hunger, these medications also slow down the process of stomach emptying. This means food stays in your stomach longer, contributing to a prolonged feeling of fullness. This mechanism is a key reason they are so effective for reducing body mass.
Originally used for diabetes treatment, GLP-1 drugs also help manage blood sugar levels. They achieve weight loss by:
- Signaling your brain to decrease hunger.
- Slowing digestion to keep you feeling full.
- Improving the body’s response to insulin.
Other Key Prescription Weight Loss Medications
While GLP-1 agonists are in the spotlight, they aren’t the only effective weight loss medications available. Several other prescription weight loss drugs have been helping people with weight management for years. These medications offer different mechanisms of action and may be a better fit for some individuals.
A knowledgeable health care provider can help you explore these alternatives, considering your specific health needs and goals for managing your body weight. Let’s dive into some of the other key players in the world of obesity medication.
Liraglutide, Phentermine, and Naltrexone-Bupropion
Liraglutide, sold as Saxenda, is another GLP-1 drug administered as a daily injection. It works similarly to weekly injectables by reducing hunger, helping patients achieve an average weight loss of 5-10% of their body weight.
Phentermine is the oldest and most widely used weight loss medication. It’s a stimulant that suppresses appetite and is approved for short-term use, though many specialists use it long-term. Naltrexone-bupropion (Contrave) is a combination pill that targets the brain’s pleasure-reward systems to decrease cravings and appetite, helping to address the mental health aspects of eating.
Like all medications, these can have side effects. Liraglutide may cause nausea and digestive issues. Phentermine can increase heart rate and blood pressure, while Contrave can cause nausea, constipation, and headache. It’s crucial to discuss these potential health problems with your doctor.
Orlistat, Setmelanotide, and Combination Therapies
Orlistat, available as Xenical by prescription and Alli over-the-counter, works differently. It’s a lipase inhibitor that blocks the absorption of some dietary fats in your gut. Undigested fat is then passed from the body. Possible side effects include oily stools, gas, and fecal incontinence, which are more common with high-fat meals.
Setmelanotide (Imcivree) is a highly specialized drug for chronic weight management in people with obesity caused by certain rare genetic disorders. Its use requires genetic testing confirmation. This highlights the move toward more personalized prescription weight loss solutions.
Combination therapies like phentermine-topiramate (Qsymia) offer another approach. This pairing enhances effectiveness for appetite suppression. The drug administration is a daily capsule. Discussing all options and their potential side effects with a healthcare professional ensures you find the safest and most effective medication for you.
Comparing Newer vs. Older Obesity Drugs
The field of weight management has seen incredible progress, leading to a clear distinction between newer and older prescription drugs for obesity. Newer medications, born from recent clinical trials, often offer greater effectiveness than their predecessors.
However, older drugs still have a place in treatment, sometimes due to cost or different side effects profiles. Understanding the key differences can help you and your provider make an informed decision. We’ll compare advancements in drug formulas as well as their effectiveness.
Advancements in Drug Formulations
One of the biggest differences between newer and older obesity drugs lies in their formulation and how they work. Older prescription drugs, like phentermine, are stimulants that suppress appetite. While effective, they were often approved only for short-term use due to concerns about side effects.
Recent advancements have led to more sophisticated drug formulation strategies. Newer drugs, like GLP-1 agonists, target specific hormonal pathways that regulate hunger and satiety. This targeted approach is designed for long-term use, treating obesity as a chronic condition rather than an acute problem.
This shift allows for more sustained management of body weight. For instance, the development of once-weekly injections and even oral versions of GLP-1 drugs has made long-term treatment more convenient and easier for patients to stick with, improving overall outcomes.
Differences in Effectiveness and Side Effects
A key difference between newer and older drugs is their effectiveness. Clinical trials have shown that newer medications like tirzepatide and semaglutide can lead to an average weight loss of 15-22% of body weight, which is significantly higher than the 5-10% typically seen with older drugs like phentermine or orlistat.
The side effects profiles also differ. While newer drugs commonly cause gastrointestinal issues like nausea and diarrhea, older drugs may carry risks of more serious side effects. For example, phentermine can increase heart rate and blood pressure. The specific differences include:
- Effectiveness: Newer GLP-1 drugs generally produce greater weight loss.
- Side Effects: Older drugs may have more cardiovascular or stimulant-related side effects.
- Mechanism: Newer drugs target hormonal pathways for a more comprehensive effect.
Ultimately, the choice depends on balancing the high effectiveness of newer drugs against the potential for side effects and the long-standing safety data of older options.
Eligibility and Guidelines for Using Obesity Drugs
Not everyone is a candidate for prescription weight loss medication. Specific eligibility guidelines are in place to ensure these drugs are used safely and appropriately. The primary factor is your body mass index (BMI), but existing medical conditions also play a crucial role.
A healthcare provider is your best resource for determining if you qualify. They will conduct a thorough evaluation to see if medication is the right step for you. Let’s review who should consider these drugs and whether being overweight, but not obese, might qualify you.
Who Should Consider Prescription Obesity Medication
Deciding to start prescription weight loss medications is a significant step that should be made with a doctor. These drugs are generally recommended for individuals who have not achieved sufficient weight loss through diet and exercise alone.
The primary guidelines for eligibility are based on body mass index (BMI) and the presence of related health problems. You may be a candidate if you meet one of the following criteria:
- A BMI of 30 or higher (defined as obesity).
- A BMI of 27 or higher with at least one weight-related health condition.
- Examples of these health conditions include type 2 diabetes, high blood pressure, or high cholesterol.
These guidelines help ensure that the benefits of the medication outweigh the potential risks. Your doctor will assess your overall health to confirm if this treatment path is right for you.
Can Overweight Individuals Qualify for Medication?
Yes, individuals who are classified as overweight but not obese can sometimes qualify for prescription drugs for weight loss. The key factor is the presence of other health issues related to their excess body weight. Being overweight is typically defined as having a body mass index (BMI) between 25 and 29.9.
Eligibility for medication usually extends to people with a BMI of 27 or higher if they also have a weight-related medical condition. These conditions can include type 2 diabetes, high blood pressure, high cholesterol, or obstructive sleep apnea.
The goal is to use medication to reduce the health risks associated with being overweight, not just to lose a few pounds. A doctor will evaluate your complete health profile to determine if the benefits of starting a weight loss medication are a sound medical decision for your situation.
How Long to Use Obesity Medications
Since obesity is considered a chronic condition, many modern medications are designed for long-term use. This approach supports chronic weight management and helps prevent weight regain after you’ve lost it. Your treatment plan will be tailored to your specific needs.
How long you stay on a medication depends on your progress, side effects, and your healthcare provider’s recommendation. It’s a journey you’ll navigate together. Let’s discuss the differences between short-term and long-term use and how progress is monitored.
Short-Term vs. Long-Term Use
The duration of obesity medication use varies. Some older drugs, like phentermine, were originally approved for short-term use, typically for 12 weeks or less. This was intended to provide a kickstart to weight loss efforts alongside diet and exercise.
However, the modern understanding of obesity as a chronic disease has shifted the focus to long-term treatment. Newer medications approved since 2012, such as semaglutide and tirzepatide, are indicated for long-term use. This continuous approach to weight management helps maintain body weight and prevent the health problems associated with weight regain.
Because obesity is a persistent condition, like high blood pressure or diabetes, stopping the medication often leads to regaining the lost weight. Therefore, many people need to take these medications indefinitely to sustain their results and manage their health effectively.
Monitoring Progress and Deciding When to Stop
Regular monitoring is a critical part of your treatment plan when using obesity medications. Your doctor will track changes in your body weight, as well as improvements in any weight-related health conditions. These check-ins help ensure the medication is working effectively.
Typically, if you haven’t lost at least 5% of your starting body weight within 12 to 16 weeks on the maximum tolerated dose, your doctor may suggest a different medication. This ensures you are on the most effective treatment for your body. The amount of lost weight is a key indicator of success.
Deciding when to stop is a complex decision made with your provider. Since obesity is a chronic disease, many modern medications are intended for long-term use to prevent weight regain. Discontinuing a drug is usually only considered if it’s not effective or if you experience intolerable side effects, taking your full medical history into account.
Expected Results and Safety Considerations
When starting an obesity medication, it’s natural to wonder about the expected results and potential side effects. The effectiveness of modern drugs can be impressive, often leading to significant weight loss and improvements in health conditions like high blood pressure.
However, safety is paramount. It’s important to be aware of the common and serious side effects and to understand that medication works best when paired with lifestyle changes. Let’s explore what you can realistically expect from these treatments.
Effectiveness of Modern Obesity Drugs
Modern obesity drugs have shown remarkable effectiveness in promoting significant weight loss. Clinical trials for GLP-1 medications like semaglutide and tirzepatide have demonstrated an average body weight reduction ranging from 15% to over 22% in some studies. This level of weight loss was previously only achievable through bariatric surgery.
This significant body weight reduction can lead to profound improvements in overall health. Patients often see better blood sugar control, lower blood pressure, and reduced cholesterol levels. Some medications have even been shown to lower the risk of cardiovascular disease in people with obesity.
The results can vary from person to person, but these advanced therapies offer a powerful tool for those struggling with obesity. They provide a new level of hope for achieving a healthier weight and reducing the burden of weight-related health complications.
Major Side Effects to Look Out For
While obesity medications are effective, they come with potential side effects. The most common side effects are often gastrointestinal. Many people experience nausea, diarrhea, vomiting, stomach pain, or constipation, especially when first starting the medication or increasing the dose. These issues are typically mild and improve over time.
However, there are also more serious side effects to be aware of. Though rare, these can include pancreatitis (inflammation of the pancreas), gallstones, kidney problems, or an intestinal obstruction. It’s crucial to discuss these risks with your doctor before starting treatment.
Pay close attention to how you feel and report any persistent or severe symptoms to your healthcare provider. Some of the major side effects to look out for include:
- Severe stomach pain that doesn’t go away
- Changes in vision
- Signs of kidney injury or gallstones
Combining Medication With Lifestyle Changes
For the best results, obesity medications should not be used in isolation. They are most effective when they are part of a comprehensive weight management plan that includes a healthy diet and regular physical activity. Clinical studies for these drugs always incorporate lifestyle modifications.
Adopting healthy eating habits and increasing your physical activity does more than just boost weight loss. It helps you build sustainable habits that support your health long after you start the medication. Strength training is particularly important to help preserve muscle mass while you lose weight.
Think of medication as a powerful tool that makes it easier to stick to a healthy lifestyle. By combining these approaches, you can maximize your weight loss, improve your metabolic health, and set yourself up for long-term success.
Conclusion
In conclusion, understanding obesity medications is crucial as they represent a significant advancement in the management of weight-related health issues. These drugs, including GLP-1 medications and others, provide various mechanisms to aid weight loss and complement lifestyle changes. It’s essential to be informed about the different options available, their effectiveness, and the potential side effects to make educated decisions about your health. Remember, the journey to achieving and maintaining a healthy weight is often multifaceted, involving medical guidance and personal commitment. If you’re considering obesity medication, don’t hesitate to reach out for expert advice and support tailored to your needs.
Frequently Asked Questions
Are GLP-1 medications effective for weight loss in obesity?
Yes, GLP-1 medications are highly effective for weight loss in people with obesity. Clinical trials show they can lead to significant reductions in body mass index by curbing appetite and improving blood sugar control. This contributes to better overall health and management of weight-related conditions.
Do I need lifestyle changes in addition to medication?
Absolutely. For the best weight management results, your treatment plan should combine medication with lifestyle changes. A healthy diet and regular physical activity work together with the drug to maximize weight loss, build sustainable habits, and improve your long-term health outcomes.
What happens if you stop taking obesity drugs?
Stopping obesity drugs often leads to weight regain. Because the treatment of obesity is a long-term process, the medication helps manage the biological factors that drive your body weight. Without it, your appetite may return to previous levels, and you may regain the lost weight, impacting related health conditions.
https://doi.org/10.1016/j.obpill.2022.100017
https://doi.org/10.1038%2Fs41573-021-00337-8
https://pubmed.ncbi.nlm.nih.gov/34518444
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10112804

